Diabetic Retinopathy
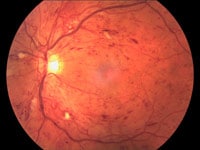 Diabetic retinopathy (DR) is the diabetic-related disease that damages your retina, causing permanent loss of vision. DR is the leading cause of vision loss across all age groups in the United States. The longer you have diabetes mellitus, either type I or type II, the higher the chances you’ll have some form of diabetic retinopathy.
Diabetic retinopathy (DR) is the diabetic-related disease that damages your retina, causing permanent loss of vision. DR is the leading cause of vision loss across all age groups in the United States. The longer you have diabetes mellitus, either type I or type II, the higher the chances you’ll have some form of diabetic retinopathy.
Diabetic retinopathy causes damage to your retina in several ways. It can cause Diabetic Macular Edema (DME), or swelling in your macula. Your macula is the part of your retina devoted to your central vision. You do not feel this swelling; rather, it causes blurry vision. The damage leads to leakage of fluid and lipids, and this leads to painless vision loss. DME can be treated with a light laser treatment to your macula, or by medicines that are administered by injection into the affected eye, similar to the treatments for “wet” age-related macular degeneration. Sometimes, your retina specialist may use a combination of treatments.
Diabetic retinopathy can also cause a vitreous hemorrhage, or a bleed into the middle part of the eye. This can cause a painless loss of vision, associated with lots of floaters and cobwebs in your vision. This hemorrhage develops when abnormal blood vessels develop in your eye in response to severe damage to your retina (Proliferative Diabetic Retinopathy). This is treated with a different laser and can also be helped by medicines that are administered by injection into the affected eye. In some cases, surgery is necessary to clear the blood and stabilize the eye.
The best way to manage diabetic retinopathy is to control your blood sugars, cholesterol and lipid levels and your blood pressure. This should be done in conjunction with your primary care physician or your endocrinologist. Additionally, close monitoring by your retina specialist allows early changes to be detected, and thus early treatments can be initiated.
